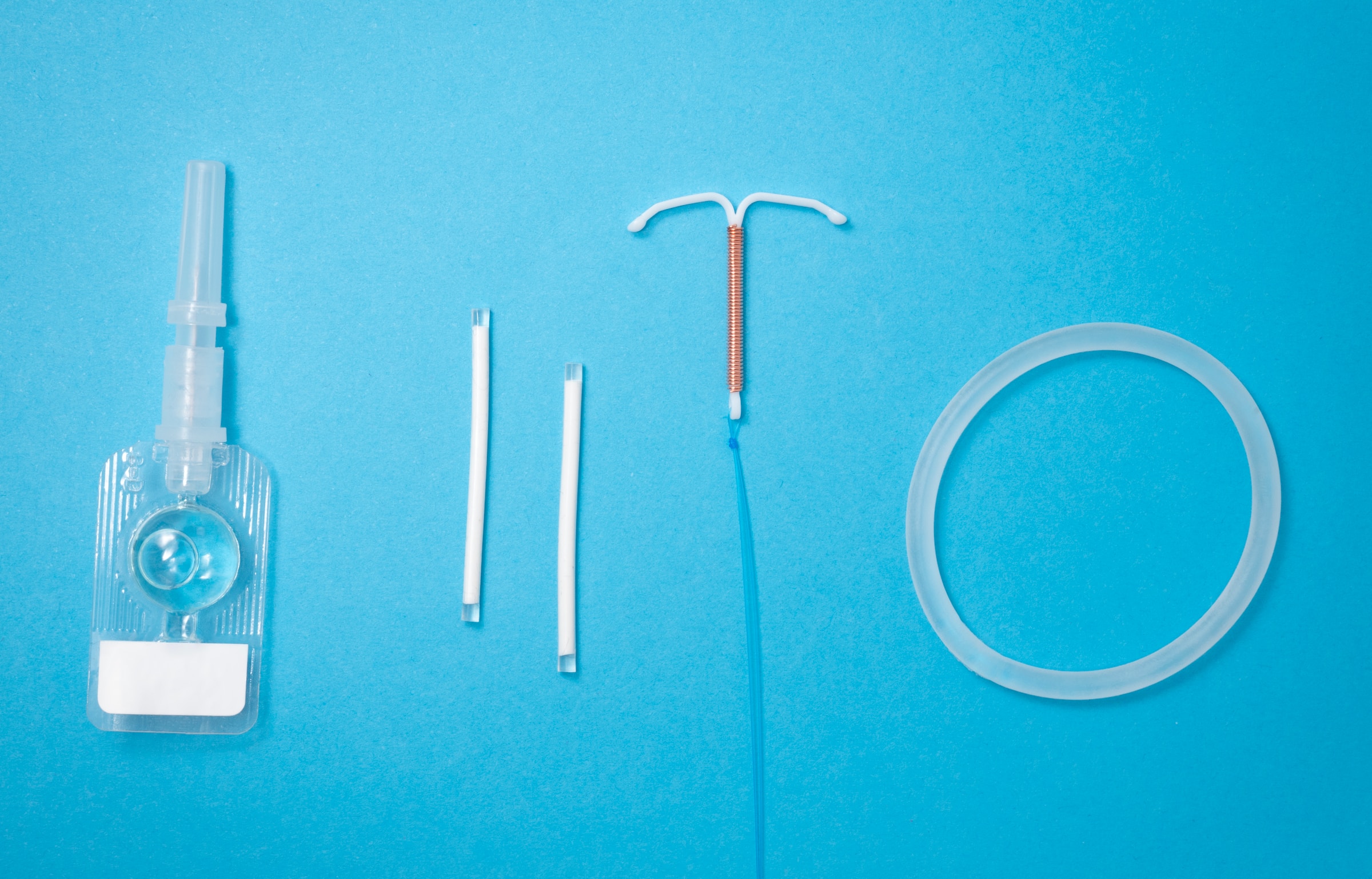
Intrauterine devices (IUDs) have surged in popularity recently as a convenient, long-term birth control method.
Modern IUDs are also highly effective, with less than a 1% chance of unintended pregnancy each year. Yet, despite significant improvements, there are still some myths around IUD safety and side effects. And when it comes to your reproductive well-being, you wouldn’t want these misconceptions to affect your decision.
If you’re considering an intrauterine device (IUD) as a contraceptive option, separating fact from fiction is crucial. The abundance of information out there can be overwhelming, especially when some myths might dissuade you from exploring this effective birth control method.
In this article, we will debunk eight common IUD myths to provide you with accurate information and help you make informed decisions about your reproductive health.
Table of Contents
Myth #1: There Is Only One Type of IUD Available
Wrong!
Just like shoes come in different styles, IUDs do, too. Modern IUDs come in two main categories based on shape: T-shaped hormonal IUDs like Mirena, Skyla, Liletta, or Kyleena, and copper non-hormonal IUDs like Paragard.
Hormonal IUDs release tiny amounts of progestin, which trims your uterine lining and thickens the cervical mucus. This makes it challenging for sperm to fertilize the egg. On the other hand, copper IUDs work by creating a hostile environment for the sperm, thus avoiding fertilization.
Within each IUD category, there are also multiple options in varying sizes and with differences in the recommended duration of effect. Understanding these options is crucial when considering an IUD, as it allows women to choose the type that aligns best with their bodies and lifestyles.
Myth #2: IUDs Are Expensive and Inaccessible
While IUDs initially cost more than some other birth control methods, their long-lasting effectiveness makes them cost-effective in the long run.
However, thanks to the Affordable Care Act, all FDA-approved contraceptive methods like IUDs are now covered at no out-of-pocket cost by private plans. Medicaid expansions have further increased accessibility and affordability for lower-income women.
While obstacles still exist for some demographics, most American women can now receive their preferred IUD at no personal cost if desired. So concerns about expense or coverage limitations should no longer deter those interested in long-acting, reversible IUD contraception.
Myth #3: IUDs Cause Severe Side Effects
You may come across anecdotes of women who experienced severe muscle spasms, heavy bleeding, or intolerable pain after IUD insertion. This fuels the fear that side effects are a given.
However, over 80% of women report being very satisfied with their IUD overall. In clinical studies, average satisfaction scores exceeded 3 out of 5 across both hormonal and non-hormonal options.
While some discomfort is normal after any new birth control method, including IUDs, it doesn’t always translate to “severe.” The most common side effects are mild and temporary, like muscle spasms, irregular menstrual bleeding, spotting, or breast tenderness. These usually subside within a few weeks or months as your body adapts to the IUD.
Serious side effects like expulsion or perforation are extremely rare. The overall IUD expulsion rate ranges from 2% to 29.8%, whereas 1 out of 1,000 IUD insertions can experience uterine perforation. However, this risk is slightly higher for women who have just given birth and are still lactating.
Regular checkups with your doctor can help catch any potential issues early and manage any lasting ones as well.
Myth #4: IUDs Are Painful to Insert or Remove
Pain is subjective. This is why you’ll hear some women say, ‘It’s as painful as childbirth,’ whereas others say, ‘I’ve dealt with worse.’
IUD insertions are minimally invasive, and doctors even use local anesthesia to reduce the discomfort. Once the IUD is inserted, you’ll feel discomfort as your body adapts to it. At worst, the pain feels similar to a heavy period cramp, but it typically subsides within a few days.
Removal is quicker and less painful than insertion. While rare, some women with non-hormonal IUDs have reported severe pain and discomfort during these procedures. There have also been thousands of Paragard lawsuit allegations claiming that the copper IUD breaks upon removal, causing severe injury.
According to Torhoerman Law, over 2,200 lawsuits have been registered against Teva Pharmaceutical and Cooper Surgical, the manufacturers and suppliers of the IUD devices. This information shouldn’t stop you from exploring your IUD options; rather, it should encourage you to stay updated with the latest IUD developments and legal proceedings.
Myth #5: IUDs Can Migrate and Get Lost in the Body
IUDs are positioned in your uterus and secured with strings that your doctor can easily check during your regular checkups.
While rare, the possibility of an IUD migrating exists, but it’s not synonymous with being ‘lost’ in the body. In most cases of displacement, women do notice changes like pain or bleeding that prompt them to get checked. So fears of an IUD dislodging without your knowledge are somewhat inflated.
To sum it up, IUDs are a safe, effective, and accessible birth control option for many women.
Don’t let misinformation hold you back from exploring this option. By debunking these myths and arming yourself with accurate information, you can make informed choices about your reproductive health and find the birth control method that’s right for you.
Remember, your body is your choice! And always consult a healthcare professional to discuss your specific needs and